Di era digital ini, permainan slot telah menjadi hiburan yang sangat digemari banyak orang. Salah satu permainan slot terbaru yang sedang populer adalah Mahjong Ways. Permainan ini telah menarik perhatian banyak pemain dengan konsepnya yang unik dan peluang kemenangan yang menggiurkan. Mahjong Ways merupakan kombinasi elemen tradisional permainan mahjong dengan fitur modern yang menarik. Dikembangkan […]
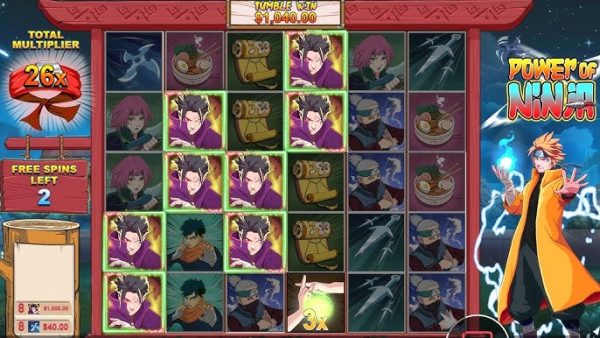
Tips Ampuh Memenangkan Jackpot Besar di Slot Online Power of Ninja dari Pragmatic
Mendapatkan jackpot besar di game slot online Power of Ninja dari Pragmatic bukanlah hal yang tidak mungkin. Dengan strategi yang tepat dan pemahaman mendalam tentang permainan, Anda bisa meningkatkan peluang kemenangan Anda. Berikut adalah beberapa tips ampuh untuk membantu Anda memenangkan jackpot besar: 1. Pahami dengan Detail Aturan dan Fitur Permainan Sebelum mulai bermain, pastikan […]
Game Slot Online Terbaru Dari Provider PGSoft Yang Mudah Jackpot
Game ini sangat seru sekali dan dibuat oleh Provider PGSoft, salah satu provider terkemuka dalam industri ini, telah meluncurkan serangkaian game slot terbaru yang menarik perhatian banyak penggemar judi online. Berikut adalah beberapa game slot terbaru dari PGSoft yang mudah jackpot dan patut untuk dicoba. 1. Gemstones Gold Gemstones Gold adalah game slot yang memukau […]
4 Game Slot Online Terbaru Dari Provider Slot JDB
Dunia perjudian online terus berkembang dengan cepat, terutama dalam industri game slot. Salah satu provider terkemuka dalam hal ini adalah JDB, yang terkenal dengan koleksi game slot inovatifnya. Dalam artikel ini, kita akan membahas empat game slot terbaru dari JDB yang patut dicoba. 1. Dragon Soar Dragon Soar adalah game slot bertema fantasi yang mengangkat […]
Review Game Slot Online Terbaru Dari Provider Advantplay Yaitu Slot Online Mace Of Hercules Mudah Menang
Jika Anda seorang penggemar game slot online, Anda pasti sudah tidak asing lagi dengan provider Advantplay. Advantplay sudah terkenal sebagai pengembang game slot online yang populer dan membuat game slot online baru dengan nama Mace of Hercules Game ini menawarkan tema yang menarik dan gameplay yang seru, serta dijamin mudah untuk menang. Advantplay: Sebuah Provider […]
Kenalan Dengan Game Slot Online Lion Dance Yang Gampang Menang Jackpot Angpao Besar
Game slot online Lion Dance adalah salah satu permainan yang populer di kalangan penggemar judi online. Game ini menawarkan kesempatan untuk memenangkan jackpot Angpao besar yang bisa membuat Anda kaya mendadak. Dengan tema yang menarik dan fitur-fitur seru, Lion Dance slot online menjadi pilihan yang menarik bagi para pemain judi online. Game slot online Lion […]
Mengenal Lebih Dekat Game Slot Online Happy Ape Yang Gampang Menang
Happy Ape merupakan slot video online yang dikembangkan oleh Habanero. Slot ini memiliki tata letak 5×3 dengan 15 garis pembayaran tetap serta berbagai fitur tambahan, termasuk hingga 36 putaran gratis, pengganda kemenangan, dan bonus unik seperti Banana Toss dan Ape Smash. Happy Ape adalah permainan slot dengan volatilitas tinggi dan RTP sebesar 96,66%. Perkenalan Habanero […]